








I’ve been wanting to share Leo’s birth story and our experience in the NICU for the past few weeks, but have hardly had time to sit down and actually write. I knew this would be a long post before I began typing it out, and I knew that it would be somewhat hard to write. Leo is a {stubborn, but} perfectly healthy baby, but the time we spent in the NICU was an emotional roller coaster, so it’s hard to relive that. However I thought this story would serve several purposes: as a therapeutic exercise for me, a great way to document everything that occurred and our feelings about everything (since at some point the details are bound to fade in our memories), and to shed light on the reasons we were in the NICU in the first place and to potentially help someone else who could end up in the same situation.
I first want to express how fortunate Dominick and I feel about Leo’s stay in the NICU. Of course it was incredibly difficult at the time and a constant emotional battle, but we were some of the lucky ones. While Leo was in the NICU for a total of 10 days, his stay was one of the shortest by far. We were in two different NICUs at two different hospitals, and we saw children that had been there for almost an entire year. Seeing other families and children that were struggling really put everything in perspective for us. While we felt incredibly sad about our situation, we knew that there were so many families who had it worse.
***
Leo’s Birth Story
FYI – this goes into detail about Leo’s birth which I was hesitant to share, but if you know me, I’m an open book 🙂 If you’re like me (especially if you’re currently pregnant or have yet to have a child), you want to know other people’s experiences so you can mentally prepare and know what to expect. If you’d rather read about our NICU experience, scroll down to the next section below.
On the morning of Wednesday, July 24th, Dom and I took our normal morning walk around our neighborhood with Lincoln before Dom had to leave for work. I remember saying to him that I thought I was going to go into labor that day. I don’t think he took me too seriously, since I had said that before haha! But I remember that morning I felt different and I thought there could be a good chance that today was the day. I was officially 39 weeks and 1 day pregnant, so I knew the baby could come at anytime, but was hoping that he or she would arrive early (our official due date was July 30th).
Dom went to work and I went about my day working from home. Since I was thinking I might go into labor that day, I knocked out a bunch of projects that I had been putting off but wanted to get done before I had our baby (thank goodness I did!). Later that afternoon my mom came over, as she and my dad flew to Austin a week before my due date. My mom and I were planning on getting our nails done in the late afternoon. After she had been at my house for a couple of hours, I told her around 3:00 p.m. that I was having contractions and thought I was probably in early labor (I had false contractions several times in my third trimester – not braxton hicks contractions, but actual contractions that were 2 minutes apart. So just because I was having contractions close together, I wasn’t actually convinced this was 100% real labor yet). My mom suggested we skip getting our nails done, but I insisted that we go (lol not stubborn at all).
While we were at the nail salon my contractions were consistently getting stronger. By the time my nails were done, I knew this was real labor – but of course my mom still had about 45 minutes left. In an attempt to get her nail tech to hurry, my mom told her that I was in labor, but she didn’t seem to fully comprehend because she did not pick up the pace (!!!). A few minutes later when the nail tech asked my mom what we had planned for afterward, my mom tried again by responding, “Probably going to the hospital!!” (lol oh, mom) The nail tech then got the hint that this was actually happening – I grant her grace because I wasn’t showing any signs of labor at all, since I was trying to just act normal and not cause a scene! Once we finally left, I made my mom drive us back to our house because I didn’t think I would be able to drive. By the time we got home, Dom was home from work and it was a mad dash to throw everything in the car and drive to the hospital.
Once we got to the hospital, I was hooked up to two monitors that tracked my contractions and baby’s heart rate. My contractions were strong and close together, but I was only 2 centimeters dilated. The hospital staff claimed they couldn’t admit me until I was 5 centimeters dilated (which my OB later told me wasn’t true), so they said they could check back again in an hour. During that hour the contractions continued to intensify to the point where I couldn’t sit or lay down, so I was standing by the hospital bed and bearing down everytime a contraction hit. When the nurses came back to check again, I was still only at a 2 so they gave me two options: 1) I could stay in that small Triage room and wait to dilate or 2) we could go home and come back in a few hours. We decided to go home because I was incredibly uncomfortable and thought that laboring at home would be better.
Fast forward an hour later when they finally discharge us and we’re headed home – I’m buckled over in the car because the contractions are so strong and I can’t physically sit still. Once we get home they continue to get worse by the second it seems and they’re hitting about every minute or two. The only thing that was even remotely comfortable was getting in the shower and letting the steaming hot water hit my lower back. Dom and I had both thought I would labor naturally and skip any pain medication for birth because I have a pretty high pain threshold and I was nervous about everything that can go wrong with an epidural (thank you birthing class). At this point, however, I was in pain that I didn’t even know existed. I was physically sick and in such severe pain that I was way past the point of crying and my body wouldn’t physically allow me to (FYI – I don’t think this is normal – most people I’ve talked to are admitted to the hospital and given pain medication way before they reach this point!).
After three hours I decided I couldn’t wait any longer so we went back to the hospital (this time I rode on all fours in the backseat because, seriously, I’m not kidding when I say I couldn’t sit down). When we arrived they checked me again and I was at a 5 thank the Lord! It was pretty much smooth sailing from there. I originally started with pain medication through an IV but was told it would only last an hour and the nurses convinced me to go with the epidural. I’m so glad I did because it saved me. I was able to sleep for a couple of hours and I was still able to move and feel my legs, which is one of the side effects I was worried about. Around 7:00 a.m. the next morning the nurses came in and woke me up to check me again, and said I could probably deliver our baby within the next couple of hours. Around 10:00 a.m. my OB came to my hospital room (along with several other doctors) to deliver our baby and about 45 minutes later, he was born! At 10:51 a.m. on Thursday, July 25th, we met our baby boy, Leonardo Joseph Puglise (Leo), weighing 7.0 lbs and measuring 19.5 inches long.
Now that it’s been 8 weeks since we had Leo, it feels like it’s been a lifetime but also that time has flown by. We are so in love with our little guy and it’s so true what everyone says – you know a completely different type of love once you have a child.



***
Leo’s NICU stay
After Leo was born, both of our parents came into our hospital room to meet him. All the doctors and nurses said he was the perfect little baby. And for the first 36 hours, he really was. He passed all of his newborn screening tests, and we were scheduled to be discharged as normal.
However the day after he was born he was taken to get a quick procedure done, which ended up making him angry, resulting in him crying hard for the first time. One of the nurses noticed when he was recovering in the nursery that when he cried, he turned blue (we were not present for this – it was about 2 a.m.). She called up to the NICU and one of the doctors came down to monitor Leo’s oxygen rate, which was dropping to dangerous levels. So they took him up to the NICU and we were notified after the fact about what had happened.
I feel like I have PTSD from those first few hours after Leo went to the NICU. That might sound dramatic, but going from having a perfectly healthy baby and expecting to be discharged the next morning, to having a random doctor barge into your room in the middle of the night to tell you that there’s something wrong with your baby who’s now in the NICU is emotionally traumatic. We weren’t told what was wrong with him (because they didn’t know), nobody told us if we could see him or not, and we were left not knowing what to do or what was going on.
After having an emotional breakdown I called my postpartum nurse into our room to get some answers and ask if we could go see Leo. Luckily we were able to go up and see him right away (even at 4 in the morning), so that is what we did. When we got up to the NICU he was hooked up to a bunch of different wires and we were told they needed to monitor him to try and figure out what was wrong.





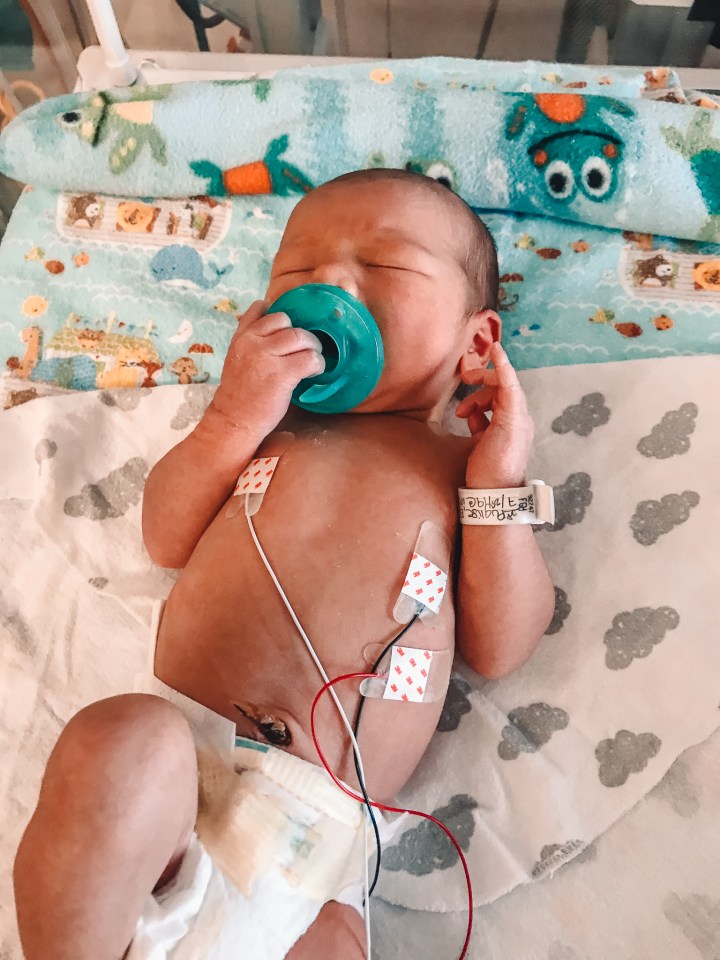
The next morning, I was discharged from the hospital but Leo was not (the worst feeling in the world). I was beyond upset at the thought of going home without Leo. Luckily the hospital I delivered at was able to secure what they call a ‘nesting room’ for us, which is a room that parents who have a baby in the NICU can stay in short-term. So while we were discharged from the post-birth unit, we just moved everything up to the NICU floor and slept in that hospital room for the next few days while Leo was still in the NICU.
The following few days had us feeling all over the place – there were highs when we thought everything was going to be okay and we would leave the hospital soon, and there were lows when it became clear that nobody could figure out what was wrong with Leo. Leo continued to have episodes where he would stop breathing when he cried, he would turn blue, and his oxygen level would drop to concerningly low levels. They continued to monitor him for 4 days in that NICU. At first we were told that it was probably a developmental delay that he would grow out of in 48-72 hours. Those 72 hours came and went and there was no improvement. With some help from family members in the medical field, we pushed for an echocardiogram to be done on his heart. Luckily that came back completely normal. But after a couple more days passed and they ran more tests, they told us they couldn’t figure out what was wrong and there was nothing else they could do. They said Leo needed to be seen by specialists, so they were going to transfer us to the NICU at the children’s hospital.
After the plan to transfer NICUs was put into place, the transfer happened pretty rapidly. The transfer unit from the children’s hospital arrived to medically transfer Leo in a transport incubator. This is when Leo’s condition kinda got real for us. We knew that Leo’s situation was not ideal, but when all of the NICU staff in the first hospital couldn’t figure out what was wrong and determined it was serious enough to transfer Leo to a better NICU, we realized that it was unlikely we would be going home anytime soon. At that point, there was no end in sight and we only wanted to bring our baby home.


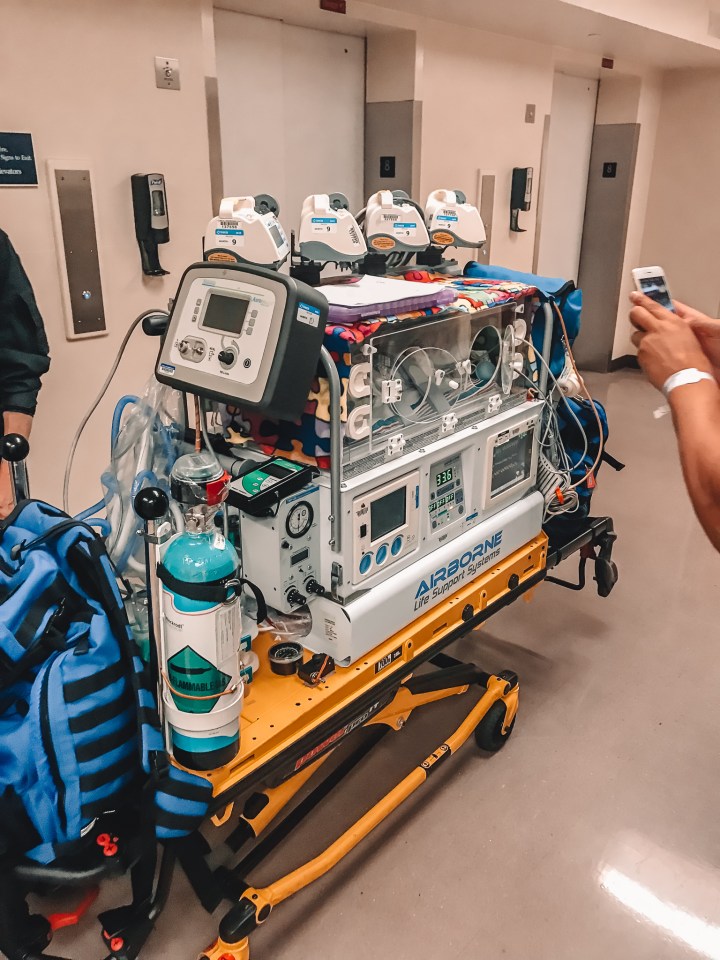

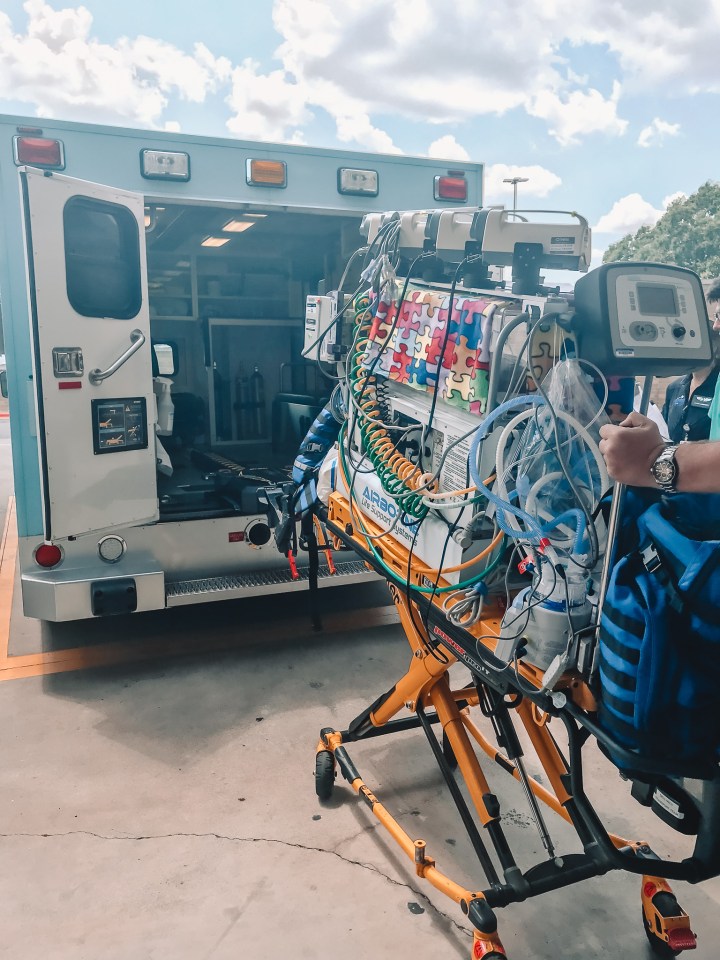

The NICU at the first hospital was set up in a pod-style, meaning that there were different ‘bays’ (aisles) that contained multiple babies, only separated by curtains if the parents were visiting and decided to close them. While this was a lack of privacy, it was also nice to be able to talk to all of the different nurses in the NICU, meet other parents, and see other babies that were also in the NICU. When we transferred to the children’s hospital, the NICU was set up much differently. Each child had his or her own room, so we were led to Leo’s individual room, which was in the back corner of the NICU. While this provided a lot more privacy, we also found it pretty isolating. After the transfer, we were only able to talk to the nurses that were specifically assigned to Leo, and we were more nervous to leave the NICU because Leo was back in a corner by himself and not surrounded by several other babies and nurses at all times. One thing they do at the children’s hospital to make the patient rooms seem more welcoming and inviting is they let the families paint the doors. So of course we had to partake!


While we were in the new NICU, we found a large electronic board on the wall in the hallway that had a list of all of the babies that were patients there along with their age and the number of days they had been there. Leo was one of the patients on the lower end, with his stay only lasting several days. This board was one of the saddest things we saw in the NICU – there were a few babies that had been there for almost a year (260+ days). Those babies had essentially been there since the day they were born. While we felt sad about Leo’s situation, this board brought us a whole new perspective and we started praying every night for all of the other babies in the NICU and their families.
Our days in the second NICU seemed much longer and they were definitely more depressing. Leo had at least one type of new procedure every day to try to determine what was causing him to turn blue when he cried. He first had a bedside scope done to look down his trachea and see if there was anything blocking his airway. When that yielded no results, the ENT (ear, nose, throat) specialist decided Leo needed to be put under general anesthesia to take the camera even further down his esophagus to either find an airway obstruction or completely rule that possibility out (a formal bronchoscopy). Again, they had to transport him down to the operating room in an incubator, and he needed to be hooked up to oxygen after the procedure and have an IV for fluids.

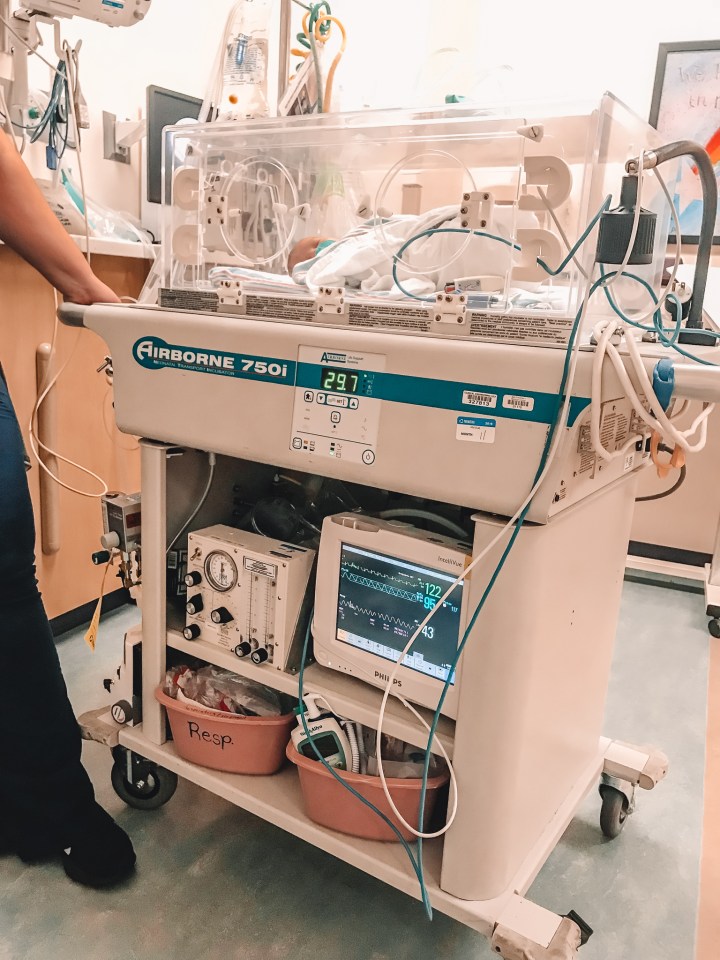
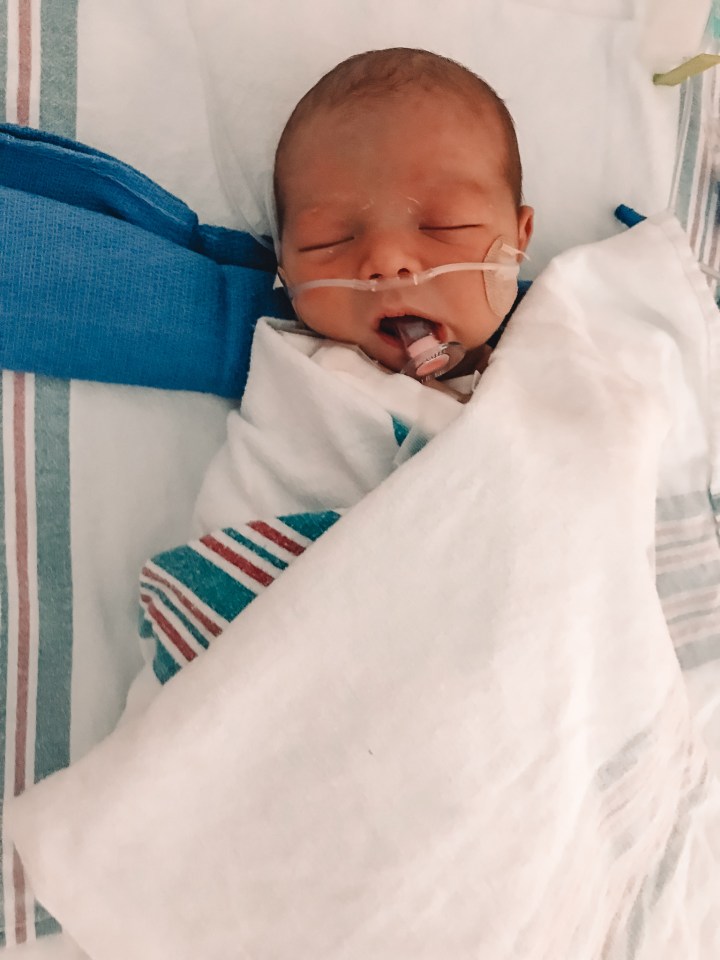

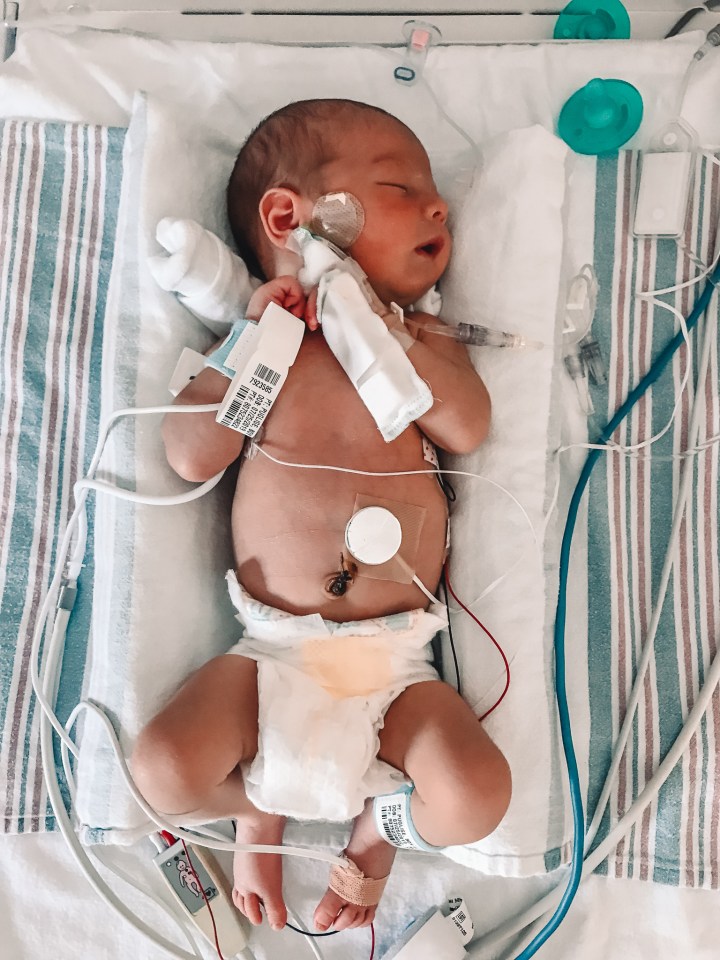

Luckily the bronchoscopy came back clear, but that meant that we still didn’t know what was causing Leo’s oxygen to drop. He was having several episodes a day, so the doctors did not want to discharge us because they still saw Leo’s condition as a risk. They continued to perform more tests on him in the following days – a second echocardiogram on his heart, an MRI on his brain, x-rays on his lungs, heart, and brain. Everything came back completely normal, but Leo was still having several episodes per day.
We were able to stay in another family room outside the NICU for the first couple of days at the second hospital, but we had to leave on the third day because a new baby was admitted to the NICU and that family was given the room. It was the first day we would have to go home to sleep, which we both dreaded, because we didn’t want to go home without Leo. We had been in the hospital for a week straight, since I had gone into labor, and going home just felt sad because we had Leo’s empty bassinet next to our bed. For the next several days, we would go home for 4-5 hours at night to sleep and head back immediately in the morning to be with Leo for as long as possible each day.

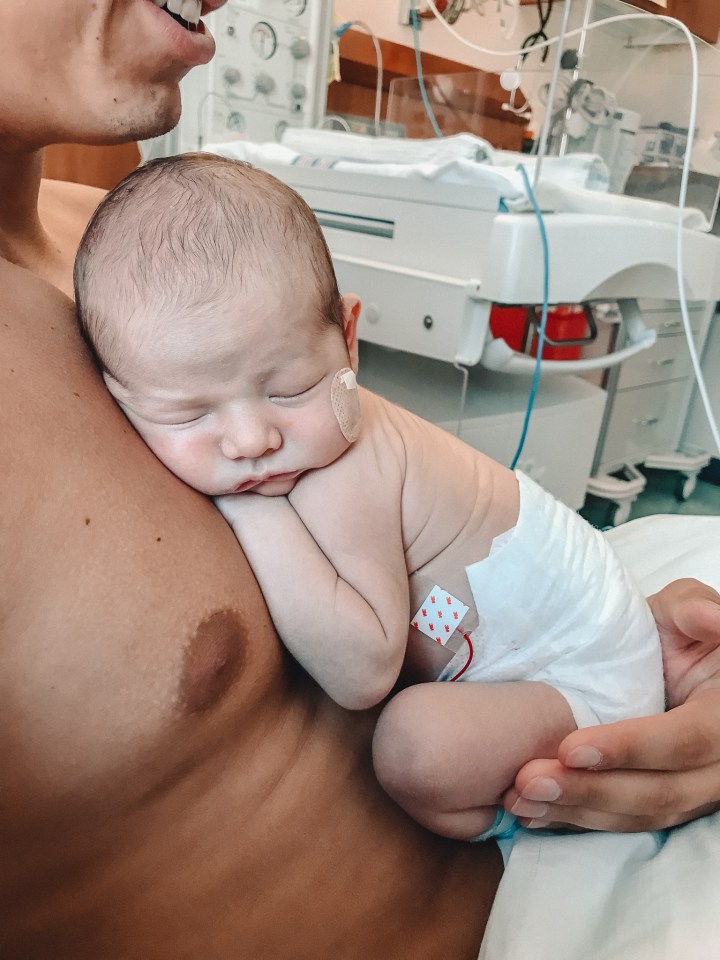


After the various specialists in the NICU had performed all of the tests they could think of on Leo, with all results coming back completely normal, it was eventually determined that Leo was most likely just holding his breath and it was a developmental issue that he would have to grow out of. Apparently there are toddlers that have similar breath-holding spells, in which they hold their breath until they pass out. However the doctors were all completely baffled by Leo because he is so little and not neurologically developed enough to mentally make the choice to hold his breath, which is why they were certain that there was something causing it. But… maybe he’s just a mini genius, after all!
With everything ruled out, Leo’s doctors still wanted to monitor his episodes and would not release us until Leo could go 72 hours without having an episode. God must have been on our side because he went from having 5-6 episodes a day to going 60 hours without a single episode. He had one minor one within the 72 hours, so luckily Leo’s neonatologist let us take him home with knowledge of how to stop his episodes if one would occur, along with a pulse-oxygen monitor that tracks his heartrate and oxygen level. So twelve days after Leo was born, we finally all went home as our new little family. It was the best feeling ever after such an emotionally draining two weeks! And we had completely forgotten what it was like to hold Leo without all of the wires attached to him :’)



Fast forward two months later, and while Leo still has episodes, they only occur once every few days and we are able to intervene and stop them from getting to a dangerous point. Leo’s pulmonologist informed us that the worst that could happen is he’ll hold his breath for so long that he’ll pass out… which we guess is better than the alternative! Luckily that has not happened and we are doing our best to ensure it never does. Still waiting on the day when he finally stops holding his breath and we stop having mini heart attacks :’) But for now we are loving our precious little boy and new life as a family of three!
A huge thank you to NICU nurses and doctors everywhere (but especially those who helped us). We wouldn’t have survived without our NICU nurses and Leo’s neonatologist, who answered our countless questions, were patient with us, stood by while we shed tears and most of all were Leo’s angels on earth.

 ‘
‘



2 thoughts on “Leo’s Birth Story + NICU Stay”